On October 1, 2022, AHCCCS updated its contracts with ACC health plans for health insurance coverage for individuals with a Serious Mental Illness (SMI) designation. In November of 2021, AHCCCS awarded select ACC health plans expanded contracts effective October 1, 2022. AHCCCS posted this announcement on its News and Updates web page.
Contract Expansion FAQs for Members, 2/22/2022
Contract Expansion FAQs for Providers, 2/22/2022

In Arizona, behavioral health has historically been a carved out benefit which has been separately managed by Regional Behavioral Health Authorities (RBHAs). Because of this structure, up to four different health care systems might be necessary for an individual with a serious mental illness (SMI) to obtain health care: the AHCCCS acute health plan for physical health services; the RBHA for behavioral health services; Medicare for, persons with SMI who are dually eligible for both Medicaid and Medicare; and Medicare Part D for medications.
Navigating the complex health care system is one of the greatest barriers to obtaining medically necessary health care. For Arizonans with SMI, obtaining needed health care has been challenging and further complicated by concerns around poor medication management and stigma, sometimes causing many individuals to forgo physical health care. Because many persons with SMI also experience co-morbidities, management of chronic diseases like diabetes or hypertension has also been poor.
To help address these issues, AHCCCS collaborated with behavioral health partners to create a more streamlined system that reduces barriers to care for members and also increases accountability of the RBHA for managing the “whole health” of persons with SMI. To carry out this new approach, RBHAs manage the delivery of physical health services, in addition to behavioral health services, to increase member engagement in obtaining medically necessary physical health services.
On April 1, 2014, approximately 17,000 members with Serious Mental Illness in Maricopa County were transitioned to a single plan, Mercy Maricopa Integrated Care, to manage both their behavioral and physical health care needs. On October 1, 2015, this model will be launched statewide through contracts with Health Choice Integrated Care in Northern Arizona and Cenpatico Integrated Care in Southern Arizona. For more information please see the resource links below.
To enhance care coordination and broaden accessibility of health care through AHCCCS, members determined to have a serious mental illness (SMI) who do not reside in Maricopa County will be enrolled in one health plan beginning October 1, 2015 for both their physical and behavioral health care needs. These members will be reassigned to one of the integrated health plans (Regional Behavioral Health Authorities (RBHAs) listed below, depending on where they live. Letters have been sent to those members whose enrollment will change to one of the integrated health plans to inform them of their new enrollment.
Members residing in the following Counties will be receiving physical and behavioral health services from Cenpatico Integrated Care beginning October 1, 2015: Cochise, Greenlee, La Paz, Pima, Pinal, Yuma, Santa Cruz, Graham and zip codes 85542 and 85192.
Members residing in the following Counties will be receiving physical and behavioral health services from Health Choice Integrated Care beginning October 1, 2015: Apache, Coconino, Mohave, Navaho, Yavapai and Gila (except zip codes 85542 and 85192).
AHCCCS has made major decisions regarding the future of RBHA service delivery, including the intention to expand the provision of services for at least one ACC plan in each GSA utilizing a Competitive Contract Expansion for the provision of integrated services for Title XIX/XXI eligible individuals determined to have SMI. The effective date for this change will be October 1, 2022
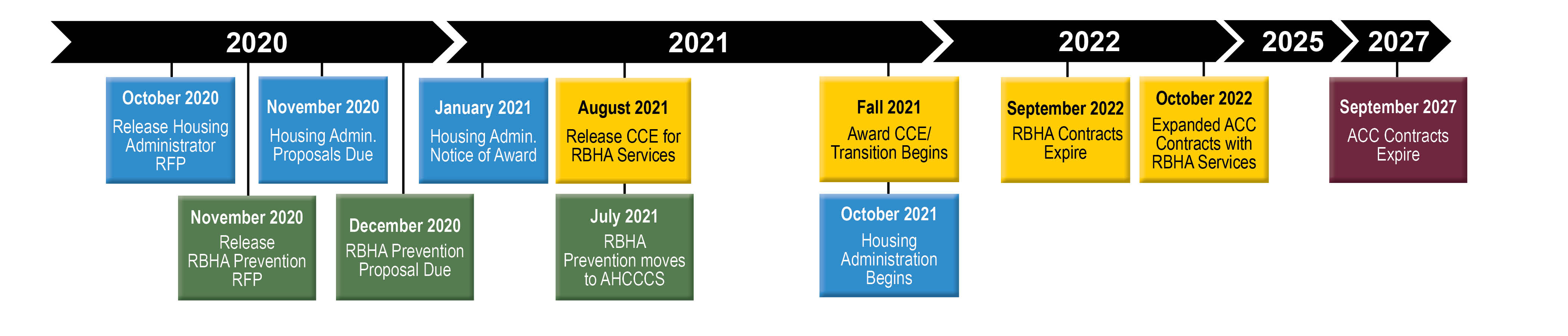
AHCCCS anticipates the timeline for Competitive Contract Expansion/ RFP activities may be as follows:
Today, American Indian members have some unique choices for Medicaid service delivery. The American Indian Health Program (AIHP) is a fee for service program delivered through AHCCCS that is responsible for integrated care for American Indian child and adult members who select AIHP and who have not been determined to have SMI. Integrated care services include both physical and behavioral health services, including services related to a CRS condition. American Indians not determined to have SMI can choose to enroll as follows:
American Indian members who are determined to have SMI are assigned to the RBHA for all services but also have a choice of staying with the RBHA or selecting AIHP for physical health services and the RBHA or TRBHA (when available) for provision of behavioral health services. American Indian members determined to have SMI are also currently permitted to be enrolled in the ACC Plan for physical health services and the TRBHA for provision of behavioral health services. or to opt out of the RBHA as specified in ACOM Policy 442 to be served by the ACC Plan for physical health services and the RBHA for behavioral health services. American Indian members can always access services from IHS/638 facilities at any time regardless of enrollment.
AHCCCS is engaging stakeholders around important system design questions and decisions that need to be made for American Indian members being served by the RBHAs and TRBHAs. Decisions need to be made regarding American Indian members continuing to have choice of enrollment with portions of their services delivered through managed care, AIHP, RBHAs and TRBHAs. The alternative is to implement change in choice for individuals determined to have SMI to be consistent with the choices for child and adult members not determined to have SMI, allowing integrated options to enroll as follows:
In order to begin to engage stakeholders around important system design questions and decisions that need to be made in order to best provide these critical services to vulnerable populations, AHCCCS released a RBHA Services RFI in February 2019. In addition, AHCCCS began presenting Community Forums in April 2019 and collected surveys to gather feedback on these changes. Additional forums and opportunities for community feedback will be posted on the Community Forums web page.
High level feedback to date from 21 written RFI responses, primarily from providers and health plans includes: