The AHCCCS Director shared an important message with the AHCCCS community that highlights the member protections during the transition to the ACC contracts.
As of October 01, 2018, AHCCCS Complete Care plans became the integrated health plans for the majority of AHCCCS members. This transition affected approximately 1.5 million members. Through this major system initiative, AHCCCS has streamlined the service delivery system for members who had previously needed to coordinate physical and behavioral health benefits through two separate health plans, while also simplifying the payment streams for the services received by members. This transition also included the flexibility for individuals designated to Children’s Rehabilitative Services to choose their ACC plan.
*With a few exceptions for members who are also eligible for CRS services, AHCCCS Complete Care will not affect: Arizona Long Term Care System (ALTCS) members, members determined to have a Serious Mental Illness, or children in foster care enrolled in the Comprehensive Medical and Dental Program (CMDP).
For Providers View all FAQs Community Meetings
Members With CRS Conditions American Indian Members
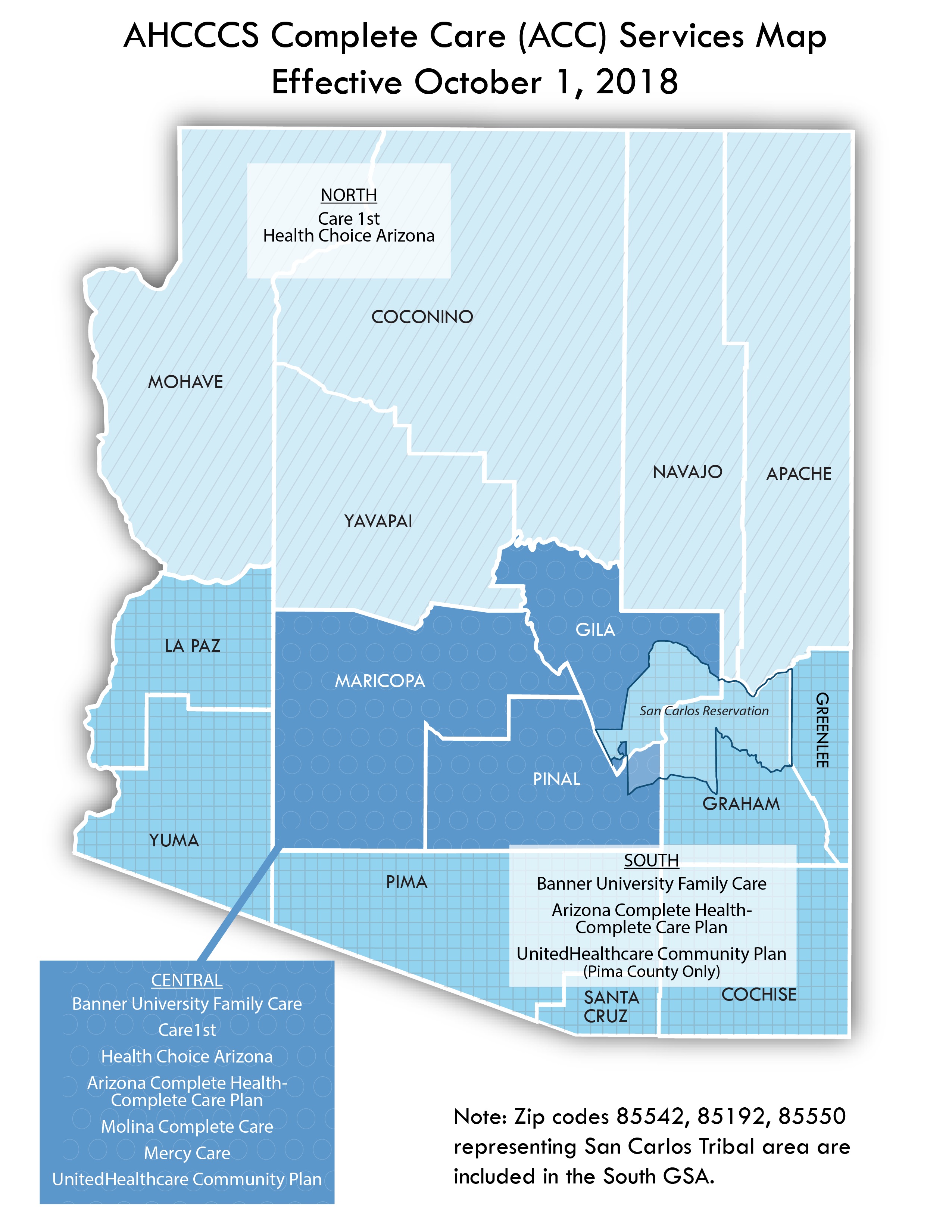
Beginning October 1, ACC plans will be available in the North, Central and South geographical service areas:
| North GSA (Apache, Coconino, Mohave, Navajo and Yavapai Counties): | Care 1st and Health Choice Arizona |
| Central GSA (Maricopa, Gila and Pinal Counties): | Banner University Family Care, Care 1st, Health Choice Arizona, Arizona Complete Health, Magellan Complete Care, Mercy Care, UnitedHealthcare Community Plan |
| South GSA (Cochise, Graham, Greenlee, La Paz, Pima, Santa Cruz and Yuma Counties): | Banner University Family Care, Arizona Complete Health, UnitedHealthcare Community Plan (Pima County only) |
Note: Zip codes 85542, 85192, 85550 (mostly in the San Carlos Tribal area) are included in the South GSA.
| ACC Health Plans | Website | Phone # |
|---|---|---|
| Care1st Health Plan | www.care1staz.com | 1-866-560-4042 |
| Health Choice Arizona | www.HealthChoiceAZ.com | 1-800-322-8670 |
| Molina Healthcare | molinahealthcare.com | 1-800-424-5891 |
| Mercy Care | www.mercycareaz.org | 1-800-624-3879 |
| Banner-University Family Care | www.bannerufc.com/acc | 1-800-582-8686 |
| UnitedHealthcare Community Plan | https://www.uhccommunityplan.com | 1-800-348-4058 |
| Arizona Complete Health-Complete Care Plan | www.azcompletehealth.com/completecare | 1-888-788-4408 |
March 5, 2018
Seven ACC health plan contracts awarded. See news announcement.
Spring 2018
AHCCCS holds public forums to explain ACC changes and choices (schedule announced in March)
June 2018
AHCCCS sends letters to members with assigned health plan information and choices
July 2018
AHCCCS members make health plan choices by July 31.
October 1, 2018
Members begin service with integrated ACC health plans
More information about contractor bidding is available in the YH19-0001 AHCCCS Complete Care Bidders’ Library